|
Dentistry Services
Dental disease doesn't just affect the teeth and cause bad breath. Besides impacting quality of life, poor oral health may lead to potentially life threatening illness such as infections of the heart valves, lungs and kidneys. As part of our dental procedures, we follow hospital protocols for anesthesia, monitoring and pain management. Your pet will receive a complete oral examination to identify and treat diseased or damaged teeth and gums. An ultrasonic scaler removes plaque and tartar and is followed by crown polishing.
Our doctors regard anesthesia and proper dental care as important events for each pet and their owners. Our hospital protocols for patients undergoing general anesthesia include a full physical examination, pre-anesthetic blood testing, intravenous catheter placement with iv fluid support, and sophisticated monitoring of blood pressure, core body temperature, respiratory and cardiac function. Anesthetic agents selected by our doctors are based on individual patient requirements and include the use of multi-modal pre-and-post operative pain management.
Examples of some types of dental care we provide include:
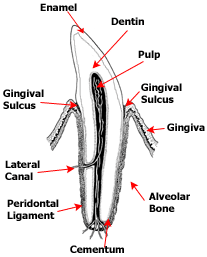
Dental Disease Grade 1
A Grade 1 disease mouth will have some plaque formation on the teeth and perhaps some mild staining. Usually there is minimal to very early gingivitis.
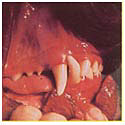 
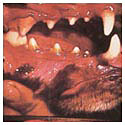
Dental Disease Grade 2
With Grade 2 disease we will notice mouth odor, brownish deposits on the back teeth, and a margin of redness along the gum line. These teeth need attention. Those brown deposits extend underneath the gums, bringing bacteria into the tooth socket. The gums are infected, and we have an important problem. At this stage, by having the teeth cleaned and doing some simple things to keep the mouth healthy, you can keep your pet comfortable and happy without a great deal of trouble or expense.
 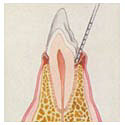
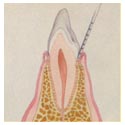
Treatment at Grade1 or Grade 2
A routine professional prophylaxis (dental cleaning and polishing, often called a 'prophy') will be discussed for pets with Grade I disease - If Grade II disease is detected, a dental evaluation with cleaning will be advised. The plaque and tartar build-up will be removed from the teeth, both above and below the gumline, with handheld and ultrasonic scalers. The teeth are then polished to remove microscopic scratches that predispose to plaque formation and calculus build-up. Each tooth and the entire oral cavity are checked for any disease. These patients receive several days of NSAID pain relief post procedure.
Dental Disease Grade 3
With Grade 3 disease, there is extensive supra and sub-gingival calculus build-up. Mobile teeth may be evident due to some loss of bone structure around the roots of the teeth. Some of the teeth will still be salvageable at this stage but some will require extraction to treat the significant periodontal disease.
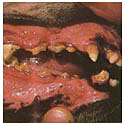 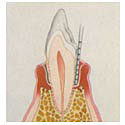
Treatment at Grade 3
A routine dental prophylaxis will not address disease of Grade 3 or 4. The mouth may be returned to manageable condition but not without effort. First we need to get the mouth cleaned up and remove the most seriously affected teeth. The diseased space under the gums where bacteria live must be thoroughly cleaned and sanitized. We then pack the area with an antibiotic gel. This material gradually dissolves over a two week period, continually releasing antibiotics. Clean and free from infection the gums are able to partially reattach to the teeth. With regular professional maintenance cleaning cleaning and home care we should be able to keep the mouth clean, comfortable and healthy. Generally this patients remain on additional oral antibiotics and pain relief (NSAID and Narcotics) for an extended period after the procedure.
Dental Disease Grade 4:
At Grade 4 Disease, basically the teeth are too far gone to save. They are loose and painful until they fall out or are extracted. Usually we can make a mouth like this comfortable and good smelling again, but only by extracting most of the teeth.
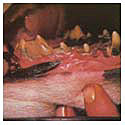 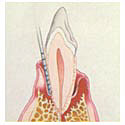
Treatment at Grade 4:
With grade 4 disease, we assess each tooth for viability. We extract any teeth deemed non-viable and clean, treat and polish remaining teeth. Generally these patients remain on additional oral antibiotics and pain relief for an extended period after the procedure.
Specialty Referral Care
There are also some Oral and Dental issues which exceed the ability of our hospital to treat in a medically appropriate manner consistent with our practice mission and philosophies - such as root canals (endodontics), artificial tooth implants, orthodontics and prosthedontics. With dental disease assessed at the Grade 3/4 stages we will mention the option of patient referral to a Veterinary Dentist for extensive dental treatment. In these instances clients interested in advanced dental care options will be offered a referral to the Board Certified Veterinary Dental Specialists at the North Carolina State University College of Veterinary Medicine.
Client Guide To Dental Estimates
Comparisons of Estimates for Dental Procedures
Please take a moment to review the information included below it just may end up saving you money, sparing you frustration and avoiding unnecessary discomfort for your pet:
Generally when our Veterinarian grades your pet's dental disease at lower levels (Grade I or II) we are providing an inclusive 'package' estimate for a set price. When our veterinarian grades your pet's dental disease at higher levels (III or IV) the estimate includes a projected range for additional tooth extraction and oral surgery time.
Examination
All anesthetic procedure patients receive a physical examination to evaluate them prior to their procedure. We assess their vital signs such as body temperature, heart rate and respiratory rate, as well as many other factors which can influence our decisions on which types of pain relief, sedation and anesthetics we choose - or, in some instances, whether to postpone the procedure.
Pre-Anesthetic Blood Testing
Prior to the use of anesthetics, your pet will have a blood sample drawn and processed by our in-house laboratory equipment. Because many anesthetic agents are metabolized and eliminated via the internal organs it is important to assess any changes from normal function which can affect how patients respond to anesthetics. These tests can alert us to organ disease, such as kidney or liver abnormalities, which are not always obvious as part of our pre-surgical physical exam. When abnormal test values are found, we may either modify our anesthetic protocols, by changing anesthetic drug choices, doses or fluid therapy, to address underlying issues or we may postpone procedures until we are better able to understand the root cause of the problem.
Intravenous Catheter and Fluid Support
As part of our standard anesthetic protocol, an intravenous catheter (IV) will be placed in a vein in your pet's leg. This catheter allows us to maintain a route of instant access to your pet's cardiovascular system for delivery of important drugs in the event an unexpected problem develops during anesthesia. In addition, your pet will receive IV fluids delivered through this catheter during and after surgery. The administration of IV fluids assists in maintaining stable blood pressure and proper blood flow to their internal organs.
Anesthetic Administration and Monitoring
Carolina Animal Hospital is serious about anesthesia. At our hospital only individuals who have completed formal educational training programs in veterinary technology and have passed stringent licensing examinations given by the North Carolina Veterinary Medical Board are employed as "Technicians".
Only a Veterinarian or a Registered Veterinary Technician, under the supervision of a Veterinarian, will ever administer anesthetics to our patients.
While under anesthesia our patients are observed by our trained staff and by sophisticated equipment which monitors blood pressure (NIBP), heart rhythm (ECG), core body temperature and oxygen levels (SPO2) in the blood stream.
Pain Management Protocol
We are also serious about pain control in our patients. Our most basic surgical and dental procedures call for the use of two forms of pain management drugs. We administer an injectable narcotic medication prior to actual anesthesia. This 'pre-med' serves two important purposes; it creates a 'warm and fuzzy' sedation which allows us to use significant less injectable anesthetic drugs to produce the desired anesthetic effect, and it helps to preempt pain responses before they even begin - which means less discomfort should be produced overall. The narcotic injection lasts for approximately six to eight hours. We also administer a non-steroidal anti-inflammatory (NSAID) drug which helps address mild to moderate discomfort, similar to high dose over the counter pain medications for humans. This drug begins to take effect shortly after administration and generally hits peak effective levels before the narcotic injection wears off. Almost all of our surgical and anesthetic patients receive additional NSAID medications for home use for several days after the procedure. We also dispense additional narcotic pain relief medications when we anticipate the level of discomfort may require more than lower level pain relief.
Amber McHugh, DVM
Colin McHugh, DVM
|